Did you know that dogs can develop a condition that is startlingly similar to Alzheimer's Disease in people? It's true. It's called Canine Cognitive Dysfunction (CCD) and a large percentage of our best friends will begin to show signs of this condition as early as 6 years old!
Diagnosis of CCD is difficult. There are sometimes changes on an MRI, but at other times all the diagnostic tests are normal. That's why we, as veterinarians, rely so much on you, the pet owner, to identify signs of this condition and begin to intervene as soon as we can.
You see, just like with Alzheimer's Disease, there is no cure for CCD. There are lots of supplements, vitamins, botanical products, and even medications that can be used to slow the progression of the disease, but no one knows how to reverse the effects.
This particular disease is one that has caused me very personal heartbreak. I had to say goodbye to the best-dang-dog-I've-ever-known, Scout, because of it.
Professor Stout Scout in his prime ...
I met Professor Stout Scout when I was a technician working at an emergency veterinary clinic in Charleston, SC. He came in the clinic as a stray and left that same night as my best friend and constant companion. He went with me to Athens, GA for vet school; to Blacksburg, VA for my internship; and all the way to Davis, CA for my residency.
It was in California that I first started to notice some of the telltale signs of CCD. Veterinarians use the acronym D-I-S-H to describe these signs.
Disorientation is common.
Interactions with their owners or other pets in the household may change
Sleep/Wake cycles are often disturbed
House-training can be lost as well
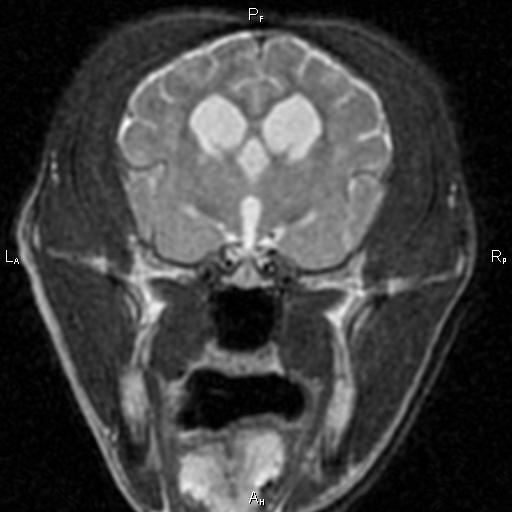
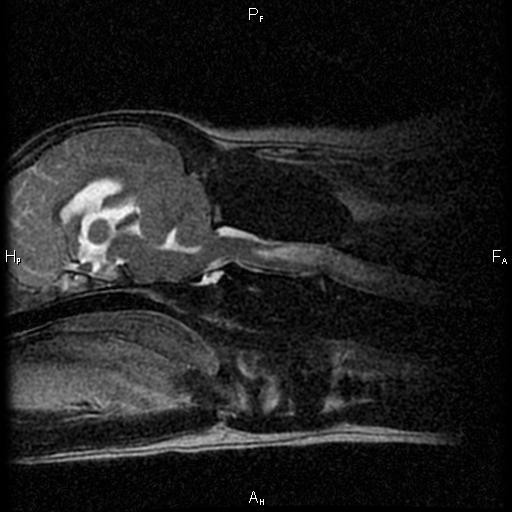
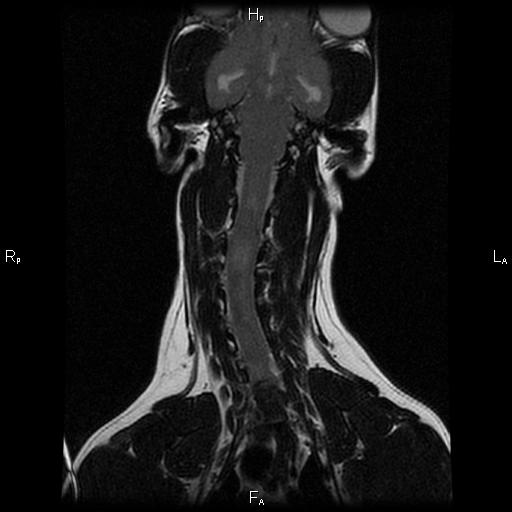
Scout started to show all these signs, and it seemed to be progressing rather rapidly. Well, I'm insatiably curious and I had to know if my buddy was starting to show signs of CCD, or if there was something else going on. Because brain tumors and other diseases can cause these signs too. So Scout had an MRI and a spinal tap at UC Davis.
Typical structural changes in a dog's brain with CCD on MRI include loss of brain tissue, dilation of the fluid-filled ventricles, and shrinkage of the interthalamic adhesion.
He must have read the same text books I was studying at the time, because he even had the structural brain changes that happen with CCD. So, he'd checked all the tick-boxes for me. I went on a search for something that might help.
I tried everything, and in the end found a cocktail of supplements and vitamins that seemed to slow his decline. I was able to get another couple of years or so with him, but CCD won in the end. Scout's quality of life declined, and I finally had to make that difficult, heartrending, and compassionate decision to help him slip off this mortal coil with all of the dignity and peace that I could muster for him.
So, if you think your older pet is starting to show signs of CCD, contact your veterinarian to have a discussion about the signs you're seeing. We still can't reverse the signs of this disease so early intervention is key...